
Find out how total joint replacement performed on an outpatient basis can get you moving.
We are one of the only outpatient total joint programs in southern California. Joint replacement is often a last resort when other treatment options have failed to provide relief. However, medical developments mean that it can be performed as an outpatient procedure.
- This method is commonly performed with less invasive arthroscopic techniques
- This method results in a more positive and productive experience with joint replacement for patients
Why Might a Joint May Need To Be Replaced?
When cartilage that normally provides cushioning for joints breaks down, it may reach a point where there’s bone-on-bone friction, which can result in disruptive joint pain. It’s a condition known as osteoarthritis, a form of arthritis associated with progressive wear of joint tissue. This is just one of several reasons why total joint replacement may be recommended.
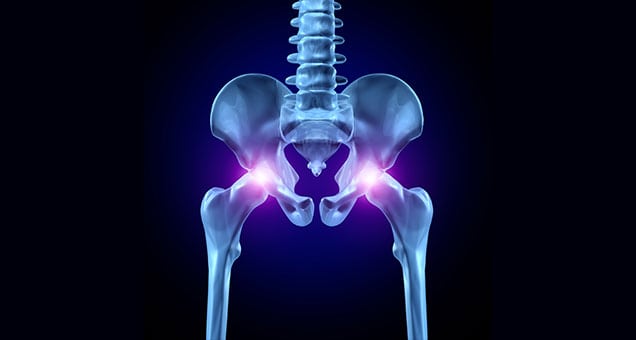
Tissues at the end of bones around joints (articular cartilage) sometimes break down from age-related wear and tear, due to a disease like arthritis that triggers inflammation around joints, a severe fracture, or an injury. Degeneration of the hip joint (avascular necrosis) sometimes causes the femoral head (the “ball” part of the ball-and-socket hip joint) to lose its blood supply and die. With knee joints, repetitive movements or multiple impacts may accelerate deterioration from tissue irritation and inflammation. Total joint replacement may become an option if a patient experiences:
- Joint pain not responding to non-surgical remedies such as physical therapy and the use of NSAIDs (non-steroidal anti-inflammatory medications)
- Discomfort around joints that’s getting progressively worse to the point where mobility is affected
- An inability to maintain a normal level of athletic performance due to chronic joint pain
- Joint-related pain that’s becoming increasingly difficult to ease or manage with other treatment options that previously helped
What’s Involved with Total Joint Replacement?
Today, surgery to replace a joint often involves arthroscopic techniques that make the experience more productive and less disruptive. Arthroscopic joint replacement can often be completed within a couple hours. Patients are usually able to go home the same day they have the procedure. The specific approach to surgery will depend on the type of joint that’s being replaced. Ball-and-socket joints, for instance, involve two parts that need to replaced, although some patients may only need to have a replacement for one part of the joint.
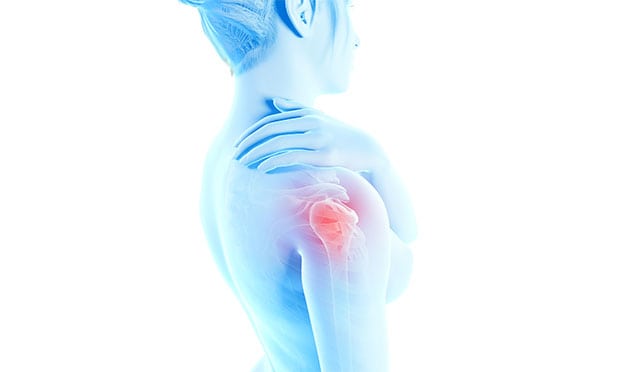
During a typical arthroscopic joint replacement, bone surfaces within the joint are removed and replaced with synthetic (artificially created) materials. The replacement parts are usually made of a type of durable, wear-resistant plastic or a mixture of various metals. Ceramic materials are sometimes used. The prosthesis is designed to match the shape of the joint it’s replacing. Some joints are mix of materials and designs. A replacement for a shoulder joint, for example, includes a polished metal ball attached to a plastic socket.
What Are Potential Benefits for Patients?
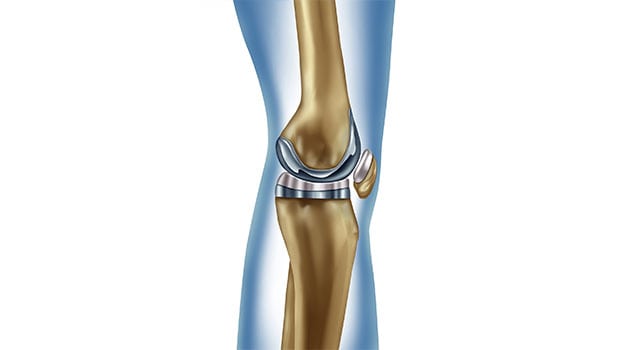
The most appealing benefit of arthroscopic joint replacement is the ability to get back to normal activities sooner. Because incisions are smaller than what’s normally required for traditional open surgery, there’s less risk of complications for patients. Precautions are also taken to avoid disturbing muscles and other soft tissues in the affected area. Even when the kneecap has to be moved for a total knee joint replacement, it’s usually done in a way that minimizes disturbance to nearby structures.
What’s Recovery Like After Joint Replacement?
Patients are encouraged to use their “new” joint soon after surgery is completed. There may be some initial stiffness and discomfort, but this will go away as recovery advances. A patient-specific schedule of physical therapy that includes exercise specific to abilities is established to help recondition muscles and get the patient used to their replaced joint.
Assistance devices such as walkers and crutches are often used until stability and flexibility improves. It’s important for patients to continue to communicate with their doctor and any pain special or physical therapist they may work with during recovery. Patients are encouraged to report anything out of the ordinary and discuss how they are functioning daily with their new joint.
Reduce your odds of needing a total joint replacement by taking steps to keep your joints and supporting tendons, ligaments, and muscles as healthy as possible. If you’re an athlete, this means stretching and doing a proper warm-up before working out, practicing, and competing. Green, leafy veggies, nuts like walnuts and almonds, and berries are among the foods you can eat that naturally reduce inflammation, which is also good for your joints. Should you experience any lingering or severe joint pain, avoid the temptation to “play through the pain” and get it checked out.
